Do Statins Cause Dementia?
The issue of dementia on statin therapy is one of the biggest barriers I see in clinical practice
I am going to start with the answer to the question of whether statins cause dementia and then provide the details backing up my answer.
The answer is: No.
Statins do not cause dementia.
If you do not read any further, you will have come away with the main takeaway of this article.
But if you are someone who thinks that statins do cause dementia and you need to see the evidence to refute that claim, then read on.
I do apologise for being direct, but this issue is one of the most frequent barriers I encounter to initiating cholesterol-lowering therapy.
A therapy that has been proven repeatedly to reduce the probability of heart attacks and strokes in multiple double-blind randomised controlled studies1.
That risk reduction is, of course, probabilistic, and it does matter what your baseline risk is and your time horizon of concern is, but….
The risk reduction is real.
FDA Warning
In 2012, the FDA issued a warning about potentially adverse neurocognitive effects of statin therapy based mostly on observational data and rare case reports2.
This warning was quickly popularised into the message:
“Statins Cause Dementia”.
But let’s look at what the FDA actually said.
“rare post-marketing reports of cognitive impairment (e.g., memory loss, forgetfulness, amnesia, memory impairment, confusion) associated with statin use. These reported symptoms are generally not serious”.
Not exactly damning and not exactly a result of rigorous controlled trial data.
One of the arguments used to support this thesis is that the brain requires cholesterol to function correctly, and lowering cholesterol to very low levels with statin therapy, or with any therapy for that matter, will cause dementia.
OK. Let’s break this down.
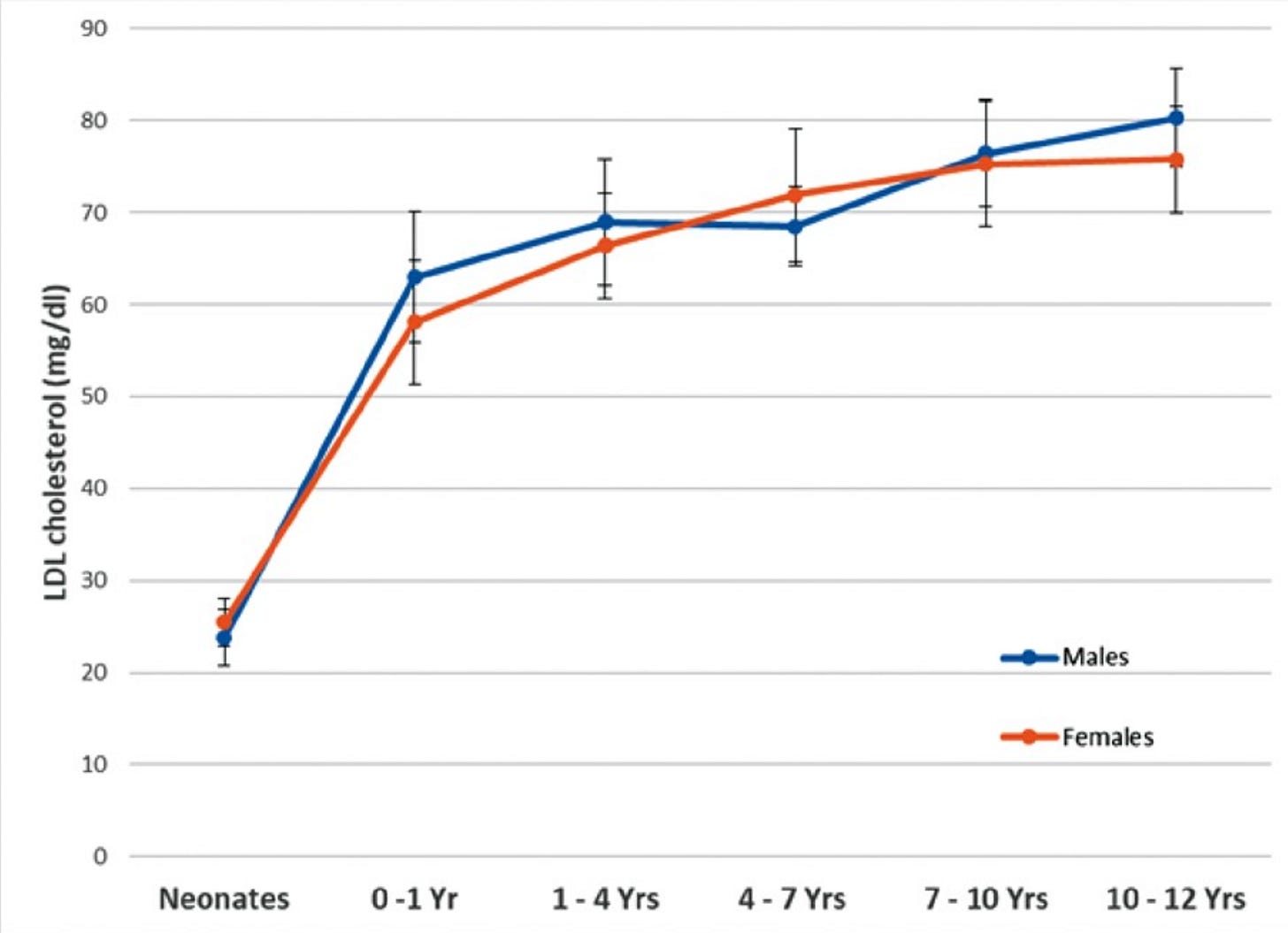
Brain development is at its peak during early childhood. At the exact same time, cholesterol concentrations are also at their lowest.
Neonates are born with an LDL cholesterol of 0.6 mmol/l (24 mg/dl)3.
Yes. That’s a zero before the decimal point.
For reference: 70 mg/dl = 1.8 mmol/l
So if, from birth to adolescence, LDL cholesterol levels are at their lowest and neural development is at its highest, it would appear that low levels of LDL cholesterol are not deleterious to brain growth and function.
Serum Cholesterol Concentration Does Not Equal Total Body Cholesterol Concentration.
The cholesterol circulating in your bloodstream represents a very small fraction of your body’s total available cholesterol.
Even if you were to reduce the circulating cholesterol in your bloodstream by 99%, you would still have more than enough cholesterol in your peripheral tissues and red blood cells4.
Additionally, the brain cells have the ability to self-generate all their own necessary cholesterol for cellular function.
Therefore, circulating serum cholesterol concentrations, which is what you see measured on a cholesterol blood test, have no bearing whatsoever on brain cholesterol concentrations.
So What Does The Data Say?
The FDA warning was issued in 2012.
We now have more than an additional decade of research on what the impact of statin therapy and aggressive cholesterol-lowering might have on cognitive function.
A study published in 2021 of almost 20,000 adults over 65 showed that those on statin therapy did not have an increased risk of:
Dementia
Mild Cognitive Impairment
Individual Cognitive Domains including global cognition, memory, language, executive function or psychomotor speed.
A 2022 systematic review and meta-analysis on statin therapy and dementia risk again showed no increased risk of dementia or Alzheimers5.
In fact, it actually suggested a potential reduction in the risk of dementia and Alzheimer’s disease, but again, this is based on observational data.
But what about VERY LOW cholesterol levels?
PCSK9 inhibitors are a relatively new therapy to lower cholesterol to very low levels, and many of the trials achieved LDL cholesterol levels routinely in the range of 0.6 mmol/l (25 mg/dl).
The levels that are typically only seen in neonates.
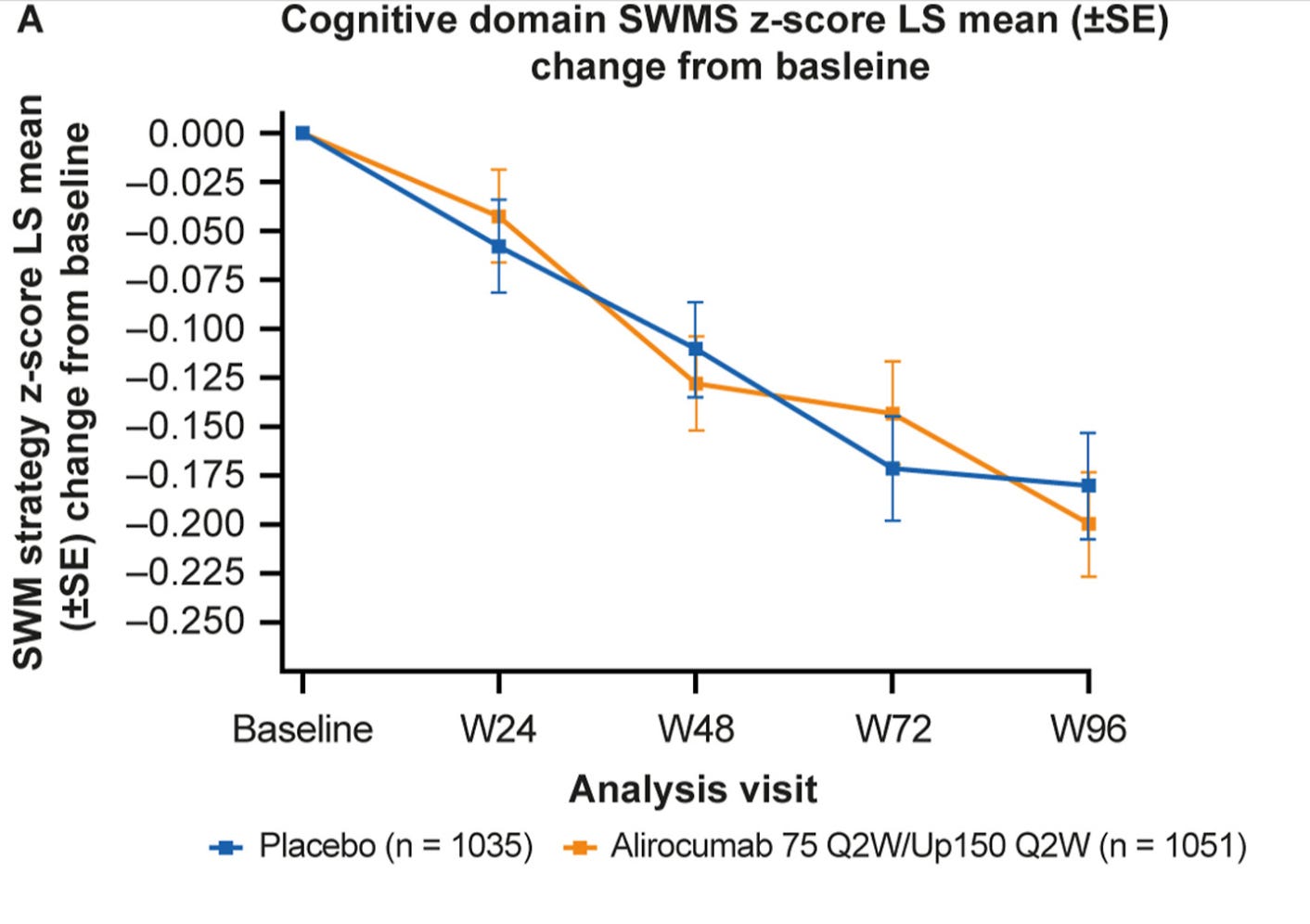
So, what happens to neurocognitive function over time?
Oh, it declines.
But no faster than someone on a placebo6.
And this is in people who mostly are already on high-dose statin therapy.
But what about younger people?
Nope. No data to support this hypothesis either7.
Trials of PCSK9 inhibitors in children aged 10 to 17 have not shown any adverse changes in neurocognitive function.
What about ‘Brain Fog’?
The term ‘brain fog’ is often used to describe a sensation of distraction, fatigue and loss of concentration on statin therapy.
While it is possible that ANY medication could cause such symptoms, the incidence of such symptoms in those on statin therapy is always subject to the dreaded ‘nocebo effect’.
Statins are often blamed for muscle aches and joint pain, but when individualised placebo-controlled data is assessed, it turns out that the absolute majority of these symptoms are not related to statin therapy alone8.
This is something I have written about before.
What About APOE?
This one requires some nuance.
Carriers of the APOE 4 gene variant are at an increased risk of late-onset Alzheimer’s dementia. They are also at an increased risk of coronary artery disease (Discussed in more detail here).
Low levels of desmosterol, a cholesterol synthesis marker, are associated with a greater risk of Alzheimer's dementia, and high-dose statin therapy can lower levels significantly in some patients9.
Some clinicians advocate reducing the intensity of statin therapy if desmosterol levels are overly suppressed. For the same level of LDL-C or APOB reduction in practice, this would likely mean adding Ezetimibe to a lower-dose statin regimen.
This approach is based on mechanistic data and has never, and likely never will be prospectively tested. Additionally, access to cholesterol synthesis biomarker testing, including desmosterol and lathosterol levels, can be challenging to obtain.
My approach for APOE 4 patients.
I use lower-dose statin therapy and add non-statin therapies earlier to get to target.
But I don’t get too worried about it.
Main Takeaways
As of today, there is no compelling evidence that, on a large scale, statin therapy or aggressive cholesterol-lowering approaches increase the risk of dementia, Alzheimer’s or cognitive impairment, even at extraordinarily low levels of LDL cholesterol.
Is it possible that a person can develop ANY SIDE EFFECT from ANY MEDICATION?
Yes. Of course, it is.
But we have to operate in the world of probabilities and not possibilities.
Are there patients who will develop ‘impaired cognition’ on statin therapy that improves when the statin therapy is stopped?
Yes.
But we usually have no idea as to whether this is all related to the nocebo effect.
My advice to patients concerned about the risk of dementia when considering starting lipid-lowering therapy and who are also at high risk of cardiovascular disease is that the benefits are much more likely to outweigh the risks.
For patients who develop ‘brain fog’, etc. I modify medications, search for alternative causes and treat them like I would any other patient on any other medication that might be causing side effects.
But when a patient says to me that they will not consider cholesterol-lowering therapy because of dementia risk, I say:
It is wonderful we live in a world where we can choose and not be compelled.
But just because we can choose does not mean we will always choose correctly.
Just make sure you are familiar with the data before you make that choice.
The effects of lowering LDL cholesterol with statin therapy in people at low risk of vascular disease: meta-analysis of individual data from 27 randomised trials. Lancet. 2012 Aug 11;380(9841):581-90.
https://www.fda.gov/drugs/drug-safety-and-availability/fda-drug-safety-communication-important-safety-label-changes-cholesterol-lowering-statin-drugs
Petra Zubin Maslov and others, High-sugar feeding and increasing cholesterol levels in infants, European Heart Journal, Volume 42, Issue 12, 21 March 2021, Pages 1132–1135,
Hellerstein M, Turner S. Reverse cholesterol transport fluxes. Curr Opin Lipidol. 2014 Feb;25(1):40-7.
Elena Olmastroni and others, Statin use and risk of dementia or Alzheimer’s disease: a systematic review and meta-analysis of observational studies, European Journal of Preventive Cardiology, Volume 29, Issue 5, March 2022, Pages 804–814, https://doi.org/10.1093/eurjpc/zwab208
Alirocumab treatment and neurocognitive function according to the CANTAB scale in patients at increased cardiovascular risk: A prospective, randomized, placebo-controlled study. Atherosclerosis. 2021 Aug;331:20-27.
HAUSER-RCT Investigators. Evolocumab in Pediatric Heterozygous Familial Hypercholesterolemia. N Engl J Med. 2020 Oct 1;383(14):1317-1327.
Cholesterol Treatment Trialists' Collaboration. Effect of statin therapy on muscle symptoms: an individual participant data meta-analysis of large-scale, randomised, double-blind trials. Lancet. 2022 Sep 10;400(10355):832-845.
Identification of a new plasma biomarker of Alzheimer's disease using metabolomics technology. J Lipid Res. 2012 Mar;53(3):567-576.


Another refreshing dose of common sense in this irrational world. Thanks Dr. Paddy!
Statins do more harm than any good!! No mention of particle size. No mention of the ratios.